丨Click on the card above to make an appointment or consult a doctor
As a dermatologist, I often encounter anxious parents in the clinic pointing to a “black spot” on their child’s cheek near the ear and asking:
Doctor, why is the child’s skin a bit black here? I pay attention to washing this area every time I wash my face, but I can’t wash it off.
This area of skin is often not painful or itchy, but it looks “dirty” and affects the appearance.
It is one of the most common causes. Especially the gray-brown area on the child’s cheek in front of the ear, it feels like fine sandpaper when touched, upon closer inspection, not only is there pigmentation, but there are also some densely packed small particles the size of pinpricks.
This is what everyone refers to as “chicken skin.”
When it comes to “chicken skin,” everyone is familiar with it. Many people’s upper arms and thighs have a rougher texture, the essence of which is hyperkeratosis of the hair follicle opening, preventing hair from growing normally.
On the cheek, especially in the “shadow area” in front of the ear, it is also a part that is prone to keratosis pilaris. With light reflection, it looks like a black area.
Keratosis pilaris is an autosomal dominant hereditary condition, many have “chicken skin,” and their children do too.
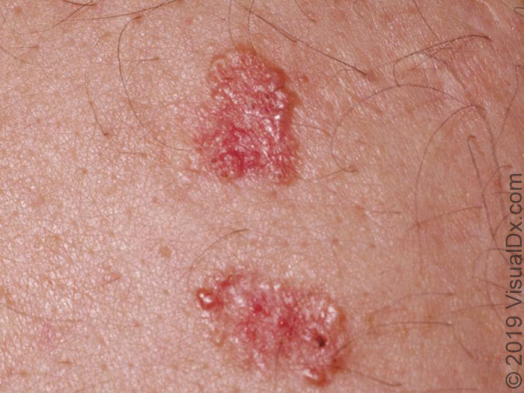
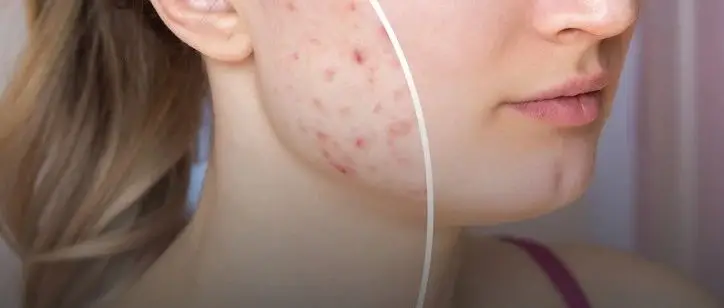
However, some children, such as older elementary school and middle school students, not only have dark skin on their cheeks, but also some redness, and some white spots like acne, affecting the child’s “beauty”.
This is not just keratosis pilaris, it also combines the erythema of telangiectasia and follicular keratotic plugs, we call it “Erythromelanosis Papulacea Follicularis,” but it is actually a clinical variant of keratosis pilaris, and it is also related to heredity.
Pigmentary demarcation lines are a clear boundary line where the skin color changes, with one side being darker and the other lighter, forming a distinct boundary, which is a physiological pigmentation difference and may be related to the migration of neural crest cells during embryonic development.
Pigmentary demarcation lines, most commonly found on the posterior lateral side of the forearm and the middle posterior side of the thigh, are more common in people with darker skin tones. On the face, the malar area and in front of the ear are also common areas.
Often occurs after skin inflammations such as eczema and dermatitis.
When the skin is inflamed, melanocytes are activated, producing excessive melanin that deposits locally, forming ill-defined patches of light to dark brown.
In addition, improper use of some topical steroid creams (too strong, too long a course) may also induce side effects such as pigmentation, local hair growth, and telangiectasia.
Caused by UV radiation, it manifests as uniform gray-brown changes on prominent facial areas (such as the malar and nasal areas) with vague boundaries. It is a normal defensive reaction of the skin to UV radiation.
For the dark areas on the child’s cheek that are not painful or itchy, the vast majority belong to benign physiological phenomena, such as keratosis pilaris, erythema papulacea follicularis, pigmentary demarcation lines, etc. Parents can check if there are corresponding characteristics to identify. These do not require special intervention, and are mainly managed with daily care and observation.
However, if there are obvious erythema, papules, accompanied by blisters, itching and pain, and other symptoms, or expanding pigmentation , it is necessary to come and let a dermatologist see whether it is serious and whether timely treatment is needed.
It should be emphasized that children’s skin is delicate, and it is not recommended to use whitening products or try folk remedies on your own.
Patient care and scientific nursing are the most reliable ways to deal with pigmentary issues on children’s faces.
Peer Review Expert Zhong Hua
Distinct Dermatologist
Ph.D. from Army Medical University, Visiting Scholar at MD Anderson Cancer Center
References
Content Editor LEE