丨Click on the card above to make an appointment or consult a doctor
Recently, as temperatures continue to rise across the country, more and more friends are visiting the dermatology department due to the recurrence of “red pimples” on the chest and back.
People are often troubled by the following:
Many red rashes the size of rice grains appear for no apparent reason, usually with white pustular changes at the top, basically painless, occasionally a little itchy.
Some friends’ rashes may spread to the neck, jawline, around the hairline, and even the scalp, lower back, abdomen, which greatly affects aesthetics.
Friends who have had similar rashes in the summer and have seen a doctor may want to answer this – is this “Malassezia folliculitis”?
Yes, this “red pimple” is different from the well-known “pimple” (acne) and belongs to a fungal infectious folliculitis. After a clear diagnosis, standardized drug treatment is needed. If you do not understand this disease, it may be treated as acne or bacterial folliculitis, such as using topical adapalene ointment, fusidic acid ointment, then the therapeutic effect will be much worse.
This issue, let’s talk about what Malassezia folliculitis is that is prone to occur in summer?
What is Malassezia?
Malassezia is a lipophilic yeast that is part of the normal flora of human skin and is a very common
commensal pathogenic fungus.
However, in areas of the skin where sebum secretion is abundant, such as when accompanied by increased sweating, Malassezia may cause folliculitis.
(Because this fungus was previously classified as Pityrosporum, it is also called “Pityrosporum folliculitis”.)
Key point, two high-incidence factors for Malassezia folliculitis:
On this basis, if there is a history of long-term oral or topical antibiotics, corticosteroid hormones, and if the overall immune status is suppressed, Malassezia folliculitis is likely to occur.
For patients
What problems can it be confused with?
Malassezia folliculitis
Usually appears on the chest, back, shoulders, all are single morphological follicular papules or pustules (see figure below) , can have mild itching, usually no significant pain.
The secondary rash areas are neck, extensor aspect of the arms , and forehead, chin, and both cheeks of the face .
However, note that Malassezia folliculitis usually does not occur in the central area of the face. And these rashes, after healing, usually do not leave much scar or color change.
Common acne (acne)
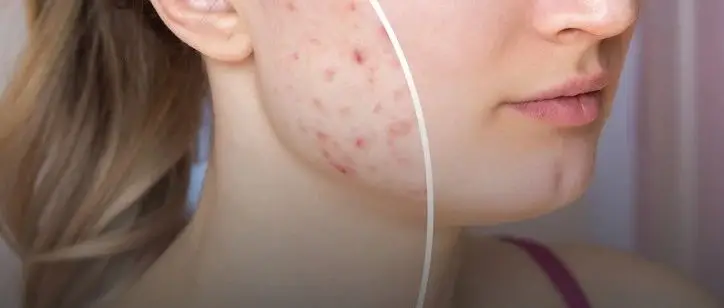
Usually appears on the forehead, nose, around the mouth, cheeks,and the jaw line and neckcan also be affected,with closed comedones, red papules, pustules, nodules as the main manifestations,may have multiple different types of rashes appear (see figure below) .
Can cause persistent red or brown acne marks for several weeks, severe cases may have depressed scars.
Bacterial folliculitis, skin boils
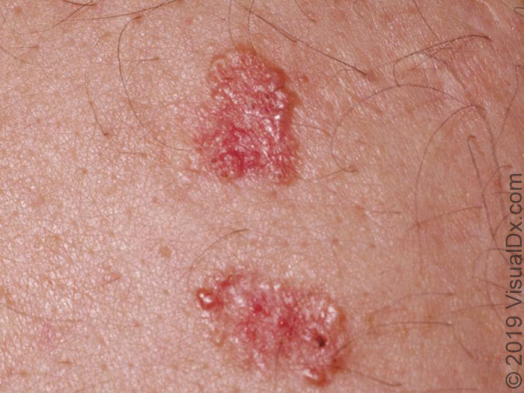
Usually appears as a red, painful swelling the size of a soybean to a pea (see figure below) , existing alone.
Early it may be hard, after 2-3 days the swelling softens, palpable fluctuation sense (gently pressing, there is a feeling like water waves shaking) , or the top gradually shows white pustular changes.
This issue requires topical or oral antibiotic treatment to ensure the rash subsides as soon as possible and to prevent the spread of infection. Usually, severe bacterial folliculitis may have deep abscesses, and in necessary cases, incision and drainage are required.
Pustular rosacea
Mainly seen in adults, typically presenting as pustules and red papules in the central area of the face.
Encountering some special irritants that worsen the condition, such as alcohol consumption, spicy food, long-term sun exposure, and heat, may cause significant exacerbation.
Perioral dermatitis
Usually characterized by red papules around the mouth, nose, or orbital area , mainly affecting young women, and the causes are usually related to local repeated use of steroids .
Diagnosing Malassezia folliculitis
What tests are needed?
For most experienced dermatology clinicians, based on the morphology of the rash, the distribution characteristics of the rash, the time of occurrence of the rash, the history of previous treatment, and physical examination, an accurate clinical diagnosis can be made and treatment can be guided.
However, for some cases where the rash is relatively rare and cannot be fully differentiated by history taking and physical examination, doctors will recommend patients to take content from one or two areas of folliculitis for a “fungal smear test” , that is, fungal microscopy.
This test is very convenient, by collecting superficial pustule scrapings to obtain smear samples, the collection process is very fast and basically painless. Put the sample on a slide with potassium hydroxide, let it stand for a few minutes, and then observe under a microscope to get the report. If budding spores and curved short mycelia are detected under the microscope, a positive result can be reported.
However, because Malassezia may normally exist in hair follicles, whether Malassezia folliculitis can be diagnosed usually also requires comprehensive fungal microscopy results by clinical doctors to make a comprehensive judgment.
How to treat and prevent Malassezia folliculitis?
As also emphasized earlier, Malassezia folliculitis is a fungal folliculitis, so oral and topical antibiotics, steroid ointments are not the right treatment, and may even worsen the condition.
The preferred treatment plan is usually:
-
Topical antifungal drugs, such as azole antifungal drugs, selenium sulfide wash, etc.
-
Oral antifungal drugs, such as fluconazole, itraconazole.
After treatment, it may not recur for several months or even years. However, the specific usage and course of treatment need to be prescribed by a dermatologist after diagnosis, which is not elaborated here.
For some people with weakened immunity, or those who are in hot and humid environments for a long time, it may still recur after treatment. Then, when early summer comes, use 1-2 times a week of selenium sulfide or ketoconazole wash to prevent recurrence (it can also be used long-term under the guidance of a doctor) .
Peer-review expert Zhong Hua
Distinct Dermatologist
Ph.D. from Army Medical University, Visiting Scholar at MD Anderson Cancer Center
References
Content Editor Falcon
Disclaimer: The purpose of the article is to provide general health information. For personal medical issues, please consult a doctor. To reprint the article, please contact: medicine@distinctclinic.com.